Progressing toward in vivo CRISPR Gene Editing in the Clinic
CRISPR news took center stage last year, with the 2020 Nobel Prize in Chemistry awarded to pioneers in the field, Dr. Jennifer A. Doudna and Dr. Emmanuelle Charpentier. The Nobel Prize win was the icing on the cake. Overall advances based on CRISPR editing tools were impressive in 2020.
For example, the application of CRISPR/Cas12 and Cas13 to the diagnosis of SARS-CoV-2 by Sherlock Biosciences and Mammoth Biosciences enabled highly specific yet rapid and simple assays for COVID-19 point of care diagnostics. Both tests, Sherlock™ CRISPR SARS-CoV-2 and SARS-CoV-2 RNA DETECTR, have received FDA Emergency Use Authorization (EUA).
CRISPR ex vivo approaches also had great success tackling inherited blood diseases. Fragoul et al. recently reported on the outcome of clinical studies sponsored by CRISPR Therapeutics and Vertex Pharmaceuticals. In these studies, two patients with mutations in the beta-globin gene (HBB) received CRISPR/Cas9 edited autologous CD34+ hematopoietic stem and progenitor cells as a novel treatment for beta-thalassemia and sickle cell diseases (CTX001, NCT03655678, and NCT03745287).
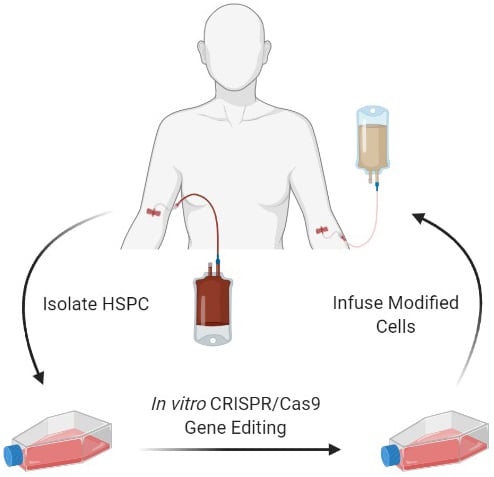
Scientists have known for some time that individuals carrying beta-thalassemia and sickle cell disease mutations benefit from elevated levels of gamma-globin and thus increased fetal hemoglobin (Sankaran and Orkin, 2013). Therefore, rather than targeting the respective disease mutations in these patients, scientists designed a CRISPR/Cas9 editing strategy enabling fetal hemoglobin re-expression in erythrocytes (Fragoul et al. 2021). The treatment proved to be life-changing for these two patients who have not required blood transfusions in a year after the CTX001 treatment.
In 2020 the US also saw CRISPR editing tools achieve a new milestone at the Clinic, with the first trial based on in vivo genome editing. The study led by Dr. Mark Pennesi at Oregon Health and Science University, and sponsored by Allergan and Editas Medicine, was designed to evaluate the safety, tolerability, and efficacy of EDT-101 administered via subretinal injection to patients suffering from the rare disease Leber congenital amaurosis (LCA), specifically LCA10.
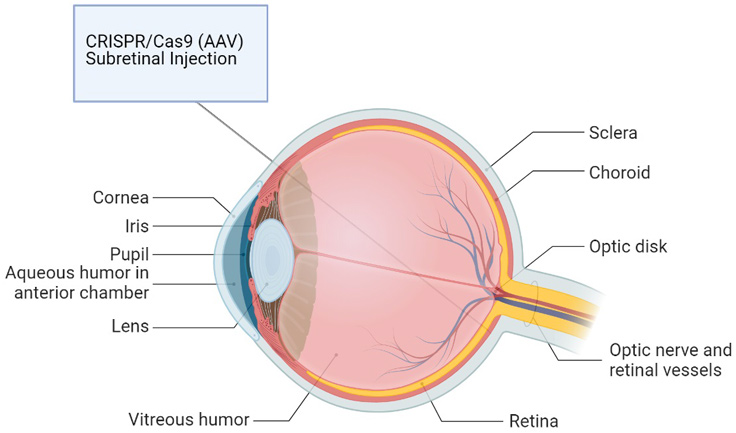
Adapted from “Anatomy of the Human Eye” by BioRender.com (2020). Retrieved from https://app.biorender.com/biorender-templates
Mutations in several genes, over 20 genes, have been linked to LCA, which affects an estimated 1/50,000 newborns who suffer from partial to complete vision loss within the first year of life. LCA10 is the most common subtype of the disease and frequently linked to the intronic A1655G mutation in the CEP290 gene. In the ongoing clinical trial, CRISPR/Cas9 and guide RNA delivered by a viral vector, AAV5, specifically targets the common A1655G mutation for repair (Maeder et al. 2019).
Continuing the progress towards in vivo therapies at the Clinic, Intellia Therapeutics’ Phase 1 study dosed its first patient at the end of 2020 with its CRISPR/Cas9 based treatment, NTLA-2001, for hereditary transthyretin amyloidosis (hAATR). This study marks another milestone, being the first CRISPR/Cas9 based therapy administered intravenously. Delivery has always been a challenge for gene editing in vivo; NTLA-2001 relies on lipid nanoparticles for liver delivery of the Cas9 mRNA and guide RNA targeting the transthyretin (TTR) gene.
Looking Forward to 2021 CRISPR Clinical Applications
For sickle cell disease, another ex vivo CRISPR/Cas9 based therapy is in the works, which directly targets the disease-causing single base mutation in the beta-globin gene. Graphite Bio’s GPH101 CRISPR/Cas9 based therapy received FDA IND clearance to start clinical studies in 2021.
Lastly, CRISPR Therapeutics announced funding from the Bill & Melinda Gates Foundation to research in vivo CRISPR/Cas9 based therapies for HIV.
Reference
Esrick, E. B. et al. Post-Transcriptional Genetic Silencing of BCL11A to Treat Sickle Cell Disease . N. Engl. J. Med. (2021) doi:10.1056/nejmoa2029392.
Maeder, M. L. et al. Development of a gene-editing approach to restore vision loss in Leber congenital amaurosis type 10. Nat. Med. (2019) doi:10.1038/s41591-018-0327-9.
Sankaran, V. G. & Orkin, S. H. The switch from fetal to adult hemoglobin. Cold Spring Harb. Perspect. Med. (2013) doi:10.1101/cshperspect.a011643.
- Like (3)
- Reply
-
Share
About Us · User Accounts and Benefits · Privacy Policy · Management Center · FAQs
© 2026 MolecularCloud



